by Jennifer Miller, Joseph Millum
BMJ Global Health, 2022;7(4):e008012 (Open access)
Abstract
New medicines and vaccines are predominantly tested in high-income countries. However, as the Covid-19 pandemic highlighted, the populations who can benefit from these interventions are not limited to these wealthier regions. One-third of novel Food and Drug Administration approved drugs, sponsored by large companies, treat infectious diseases like tuberculosis and HIV, which disproportionately affect low-income and middle-income countries (LMICs). The medicines for non-communicable diseases (NCDs) are also relevant to LMIC health needs, as over three-quarters of deaths from NCDs occur in LMICs. There are concerns clinical trial data may not extrapolate across geographical regions, as product effectiveness can vary substantially by region. The pentavalent rotavirus vaccine, for example, had markedly lower efficacy in LMICs. Efficacy variations have also been found for other vaccines and drugs. We argue there are strong ethical arguments for remedying some of this uneven distribution of clinical trial sites by geography and income. Chief among them, is that these disparities can impede equitable access to the benefits of clinical research, such as representation in the evidence base generated to guide prescribing and use of medicines and vaccines. We suggest trial site locations should be made more transparent and for later stage trials their selection should be informed by the global distribution of disease burden targeted by an experimental product. Countries with high prevalence, incidence, severity or infection transmission rates for targeted diseases should have real opportunities to engage in and enrol their populations in trials for novel medicines and vaccines.
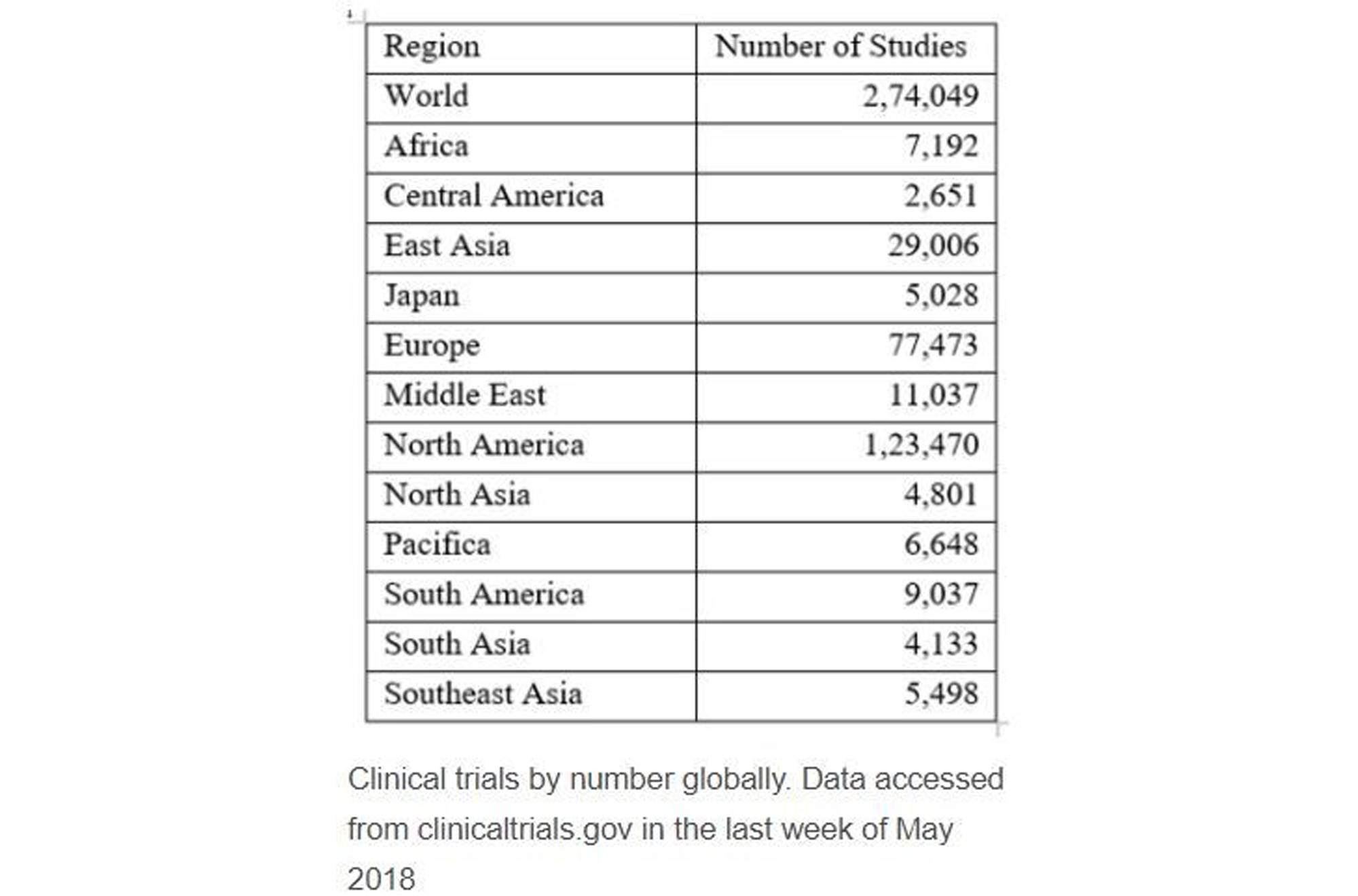
INFOGRAPHIC: Africa hosts very few clinical trials, The Conversation, by Swapan Kumar Patra, 4 June 2018



